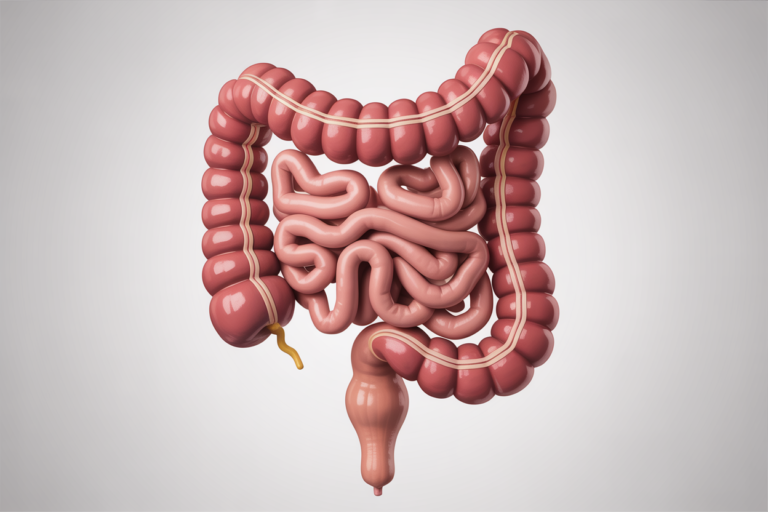
Most people think digestion ends in the stomach. In reality, one of the most important stages happens later inside the large intestine, also called the colon. This is where your body reclaims water, balances electrolytes, supports gut bacteria, and converts waste into stool for elimination.
When the large intestine is not functioning properly, the effects are not limited to constipation or diarrhea. It can influence immunity, metabolism, inflammation levels, and even mental well-being through the gut-brain axis.
For many patients across Bengaluru and India, symptoms like bloating, irregular bowel movements, or abdominal discomfort are often ignored until they become severe. Understanding how the large intestine works helps you recognize when something is normal and when it needs medical evaluation.
This guide explains the large intestine in simple terms – its anatomy, functions, common disorders, warning signs, diagnostic tests, and ways to maintain colon health.

The large intestine is the final section of the digestive tract. It is a muscular tube about 5 feet long that frames your abdomen. It receives semi-digested material from the small intestine and processes what remains.
Unlike the small intestine, which focuses on nutrient absorption, the colon focuses on fluid balance and waste management.
Understanding colon anatomy helps explain where pain or disease may occur.
The starting pouch where material enters from the small intestine. The appendix is attached here and acts as a reserve for beneficial bacteria.
Moves upward on the right side of the abdomen. Major water absorption begins here.
Crosses the upper abdomen. Active bacterial fermentation occurs in this section.
Moves down the left side. Stool becomes more formed and concentrated.
An S-shaped segment that stores stool before it moves into the rectum.
Final storage area that triggers the urge to pass stool.
Your body sends about 1-2 liters of fluid daily into the colon. The large intestine reabsorbs most of it.
This is why bowel movement speed matters.
2️. Fiber Fermentation and Gut Bacteria Support
The colon contains trillions of microbes — your gut microbiome.
They ferment fiber and resistant starch to produce:
Low fiber diets reduce this protective effect. Traditional Indian foods like millets, dals, and fermented foods naturally support this process.
Colon movement is slower and patterned:
If nerve or muscle coordination fails, patients may develop chronic constipation or incomplete evacuation.
Specialized motility testing is often required in such cases rather than repeated laxative use.
The large intestine is the main habitat of gut bacteria. These organisms influence:
Methane-producing microbes are strongly linked to constipation-predominant IBS. This is why breath testing is now used in advanced gastroenterology centers.
Microbiome imbalance (dysbiosis) is increasingly seen in urban Indian populations due to:
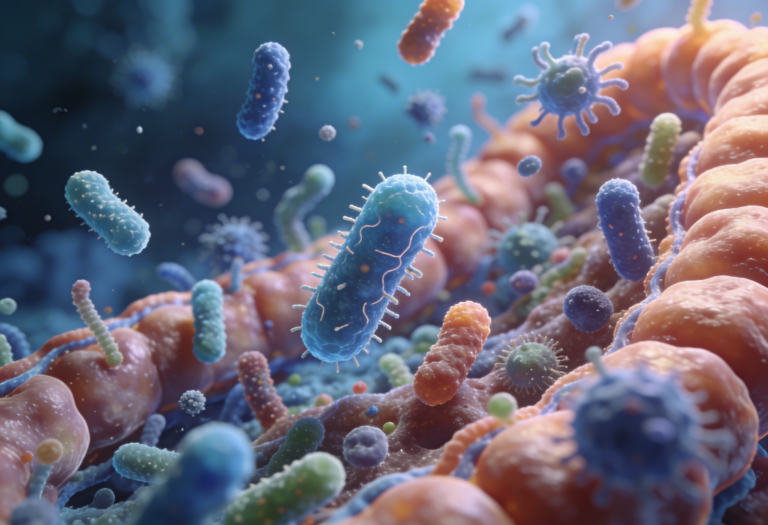
One of the biggest drivers of constipation and colon disease risk.
Food additives may damage the gut lining and mucus barrier.
Fiber without water worsens stool hardness.
Destroys beneficial gut bacteria.
Alters gut-brain signaling and motility patterns.
A hidden cause of constipation where muscles fail to relax during defecation.
Raises risk of inflammatory bowel disease and colorectal cancer.
These often relate to IBS, motility issues, or microbiome imbalance.
These require prompt medical evaluation:
Patients in South Bengaluru increasingly present late because symptoms are tolerated too long. Early colon evaluation improves outcomes significantly.
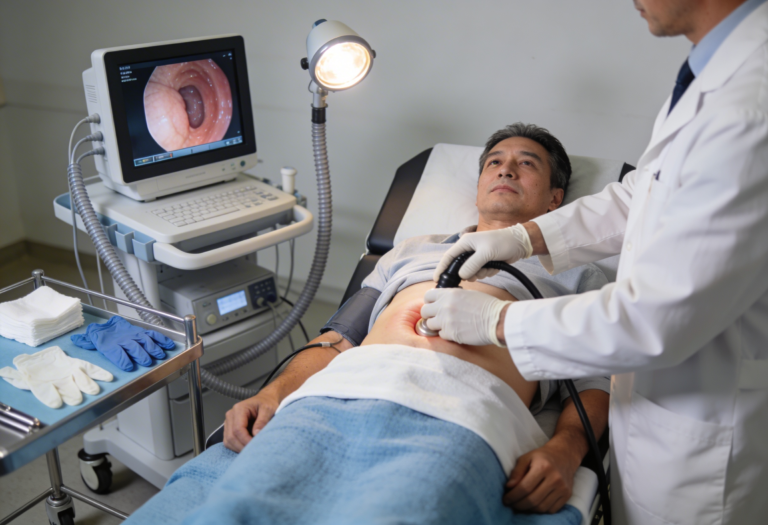
Modern gastroenterology uses both structural and functional tests.
Gold standard test to examine the entire colon.
Detects:
Also allows biopsy and polyp removal.
Used to detect:
Very useful in bloating and unexplained constipation.
Measures rectal and sphincter muscle coordination.
Critical for:
Available mainly in specialized gut motility centers.
Microbiome mapping – bacterial composition
Functional disorder with pain and bowel pattern change. No structural damage but major quality-of-life impact.
Types:
Includes:
Autoimmune inflammation that requires long-term specialist care.
Small pouches in the colon wall. Can become infected (diverticulitis).
Often starts as a polyp. Preventable with screening colonoscopy. Screening is strongly recommended after age 45 or people with earlier family history.
Treatment depends on the root cause – not just symptoms.
Primary treatment for pelvic floor constipation – more effective than repeated laxatives.
Many advanced gut clinics, including Gut Health Doctor programs, use structured gut restoration models:

ICMR guidelines recommend 30-40 grams fiber daily for adults.
Consider consultation if you have:
Specialist evaluation helps distinguish IBS from inflammatory or structural disease – which changes treatment completely.
Mid-stage evaluation prevents long-term complications and repeated trial-and-error treatments.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.