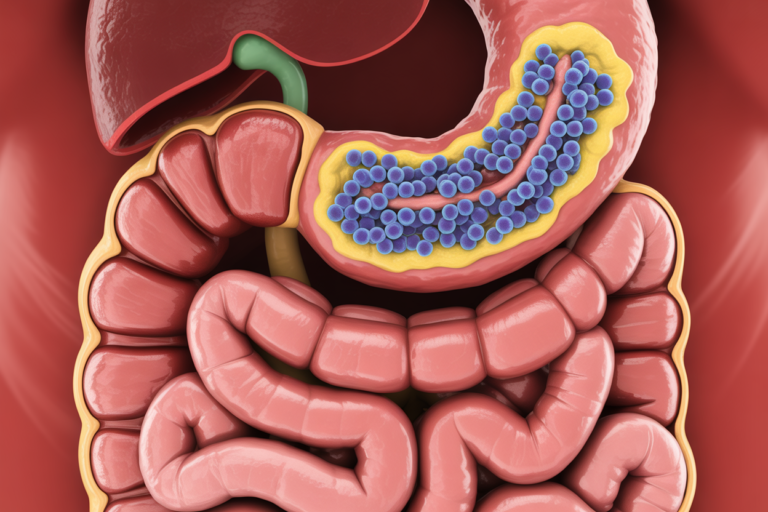
The gut lining is a thin layer of specialized cells that lines the inside of your intestines. It forms the boundary between what is inside your digestive tract and what is allowed into your bloodstream.
Technically, the inside of the gut is considered “outside” the body until nutrients cross this lining.
The gut lining must perform two opposite jobs at the same time:
This selective barrier function is what keeps your internal system protected.
The intestinal lining covers roughly 30 to 40 square meters of surface area — comparable to a small sports court. It is one of the largest interfaces between your body and the external environment.
It is also highly dynamic:
Because renewal is rapid, the gut lining can repair but only if damaging triggers are removed and proper nutrients are available.
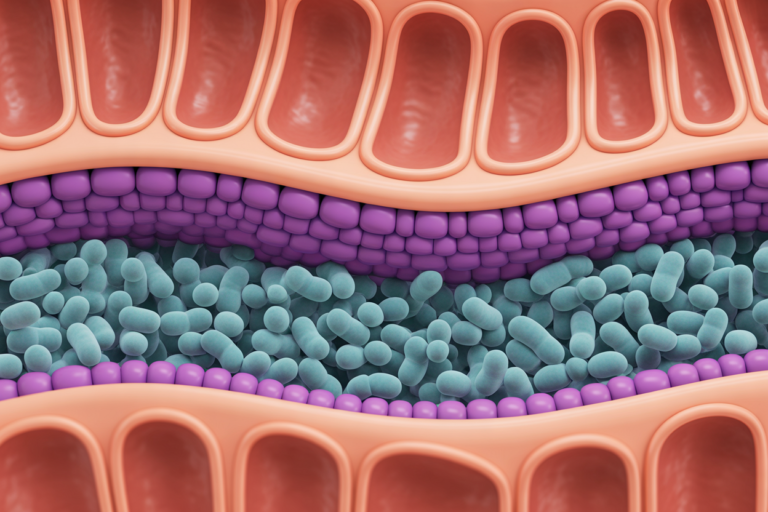
The gut barrier is not a single wall. It is a multi-layer defense system.
Beneficial bacteria live on top of the gut lining and provide first-line defense.
They:
Traditional Indian fiber-rich diets historically supported this layer, but refined diets reduce this protection.
A gel-like mucus coating sits above the cells.
It:
Low fiber intake, stress, and additives can thin this layer.
This is a single layer of tightly packed intestinal cells.
Between these cells are tight junctions – microscopic gate structures that open briefly to allow nutrients through and then close.
These tight junctions are the core of barrier control.
Directly beneath the lining sits gut immune tissue.
It contains:
If unwanted substances cross the barrier, this immune layer activates inflammation.
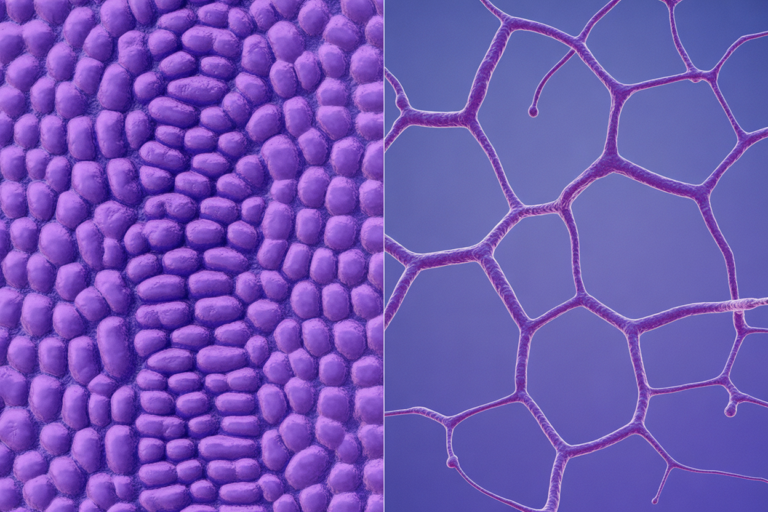
In medical science, the correct term is intestinal hyperpermeability.
It means the tight junction gates are not closing properly, allowing larger molecules to pass through.
This is measurable in research and clearly established in conditions like:
The popular term “leaky gut syndrome” is broader and sometimes overused online, but barrier dysfunction itself is medically real.
A key regulator protein called zonulin controls tight junction opening.
Triggers include:
Short opening is normal. Prolonged opening causes problems.
Specialist programs such as GutHealthDoctor evaluate these triggers instead of assuming all symptoms are acid or IBS alone.
Modern lifestyle factors are major contributors.
These disrupt mucus and microbiome balance.
Stress hormones:
This explains why anxiety and digestive symptoms frequently coexist.
Common medicines can weaken the barrier:
At centers like Arka Multi-Speciality Hospital, medication history is routinely reviewed during digestive evaluation.
Poor sleep:
Shift workers show higher rates of gut dysfunction.
Symptoms are often mixed and multisystem.
Because immune activation spreads beyond the gut.
These are not functional symptoms and need specialist testing:
Hospital gastroenterology evaluation – such as at Arka Multi-Speciality Hospital is recommended in these cases.
Standard scopes cannot see microscopic permeability, but they rule out major disease.
Programs led by Dr. Gaurang Ramesh at GutHealthDoctor often combine structural and functional testing when symptoms persist despite normal scans.
Repair follows a staged approach, not random supplements.
Evidence-supported nutrients include:
If symptoms are persistent, structured medical guidance is more effective than trial-and-error supplement use.
Consult a specialist if:
Patients in Bengaluru and across India often seek structured barrier and microbiome evaluation through GutHealthDoctor under Dr. Gaurang Ramesh and gastroenterology teams at Arka Multi-Speciality Hospital.
Is leaky gut medically real?
Intestinal permeability is medically real and measurable.
Can it be tested?
Yes via specialized functional tests.
How long does repair take?
Typically weeks to months depending on severity.
Is gluten always harmful?
No, but it increases permeability temporarily in everyone.
Does stress damage the gut lining?
Yes, proven via immune and tight junction effects.
Can probiotics worsen symptoms?
In SIBO, yes testing first is important.
Best Indian foods for gut lining?
Fermented foods and fiber-rich traditional foods.
Does fasting help gut repair?
Short overnight fasting windows support gut cleaning cycles.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.