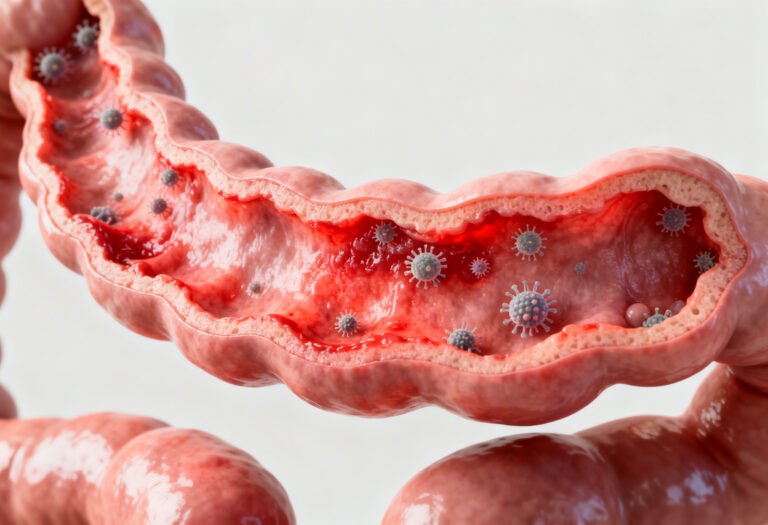
Gut inflammation is one of the most overlooked health issues in modern India. Many patients experience persistent bloating, fatigue, loose stools, food intolerance, or unexplained skin flare-ups without realizing that the root problem may be chronic inflammation in the gut lining.
Inflammation inside the gastrointestinal tract is not always dramatic. In early stages, it can be subtle and easily dismissed as “acidity,” “IBS,” or simple digestive weakness. However, when left unchecked, chronic gut irritation can progress into more serious conditions such as Inflammatory Bowel Disease, autoimmune disorders, or long-term nutrient deficiencies.
In cities like Bengaluru, changing food patterns, antibiotic overuse, stress-heavy work culture, and processed diets are contributing to a rise in inflammatory gut conditions. Early evaluation can prevent structural damage and long-term complications.
Inflammation is the immune system’s protective response. In the gut, it occurs when the intestinal lining detects harmful bacteria, toxins, undigested food particles, or infections.
Acute inflammation is normal. For example:
However, chronic gut inflammation occurs when the immune system remains activated for months or years. Instead of protecting the body, it begins damaging the intestinal barrier itself.
This ongoing immune activation can lead to:
This is often referred to in research as increased intestinal permeability, commonly called “leaky gut.”
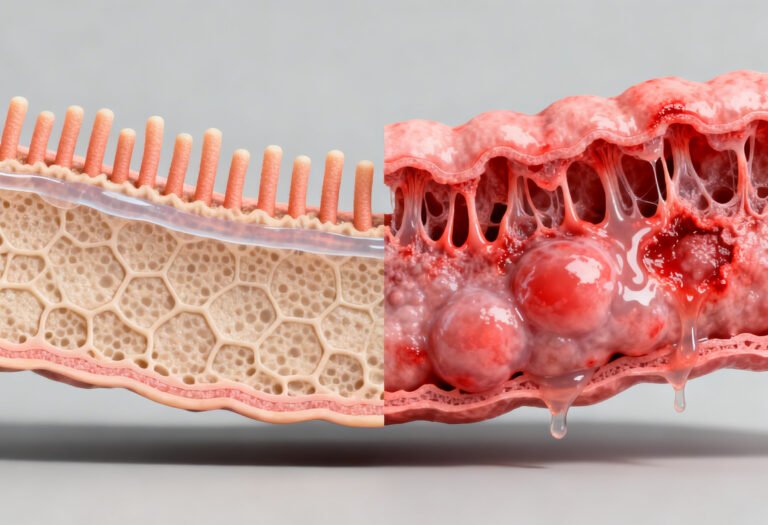
The intestinal lining is only one cell thick, yet it performs a highly complex job.
It must:
Key components include:
When this barrier weakens, bacteria and toxins enter deeper tissues, triggering inflammation.
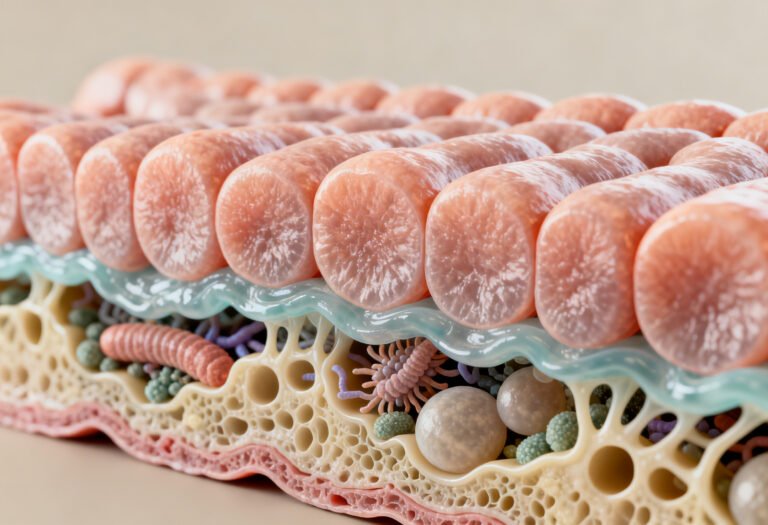
Gut inflammation rarely has a single cause. It usually results from multiple stressors acting together.
Diets high in:
can disrupt tight junction integrity and alter microbiome diversity.
Stress activates the sympathetic nervous system and increases cortisol levels. This reduces blood flow to the gut and slows mucosal repair. Over time, stress contributes to chronic gut irritation through the gut-brain axis.
Repeated antibiotic exposure disrupts beneficial bacteria, allowing opportunistic organisms to dominate.
Frequent use of painkillers such as ibuprofen can directly damage the intestinal epithelium.
Past bacterial or parasitic infections can leave behind a hyper-reactive immune response.
Conditions like Crohn’s disease and Ulcerative Colitis have genetic components, though environmental triggers often determine activation.

Many patients overlook early symptoms.
Chronic bloating not relieved by dietary adjustments may indicate mucosal irritation or SIBO.
Long-standing loose stools require evaluation.
This is a red flag and should never be ignored.
Especially if it worsens after eating.
Inflammatory cytokines can cause systemic tiredness.
Linked to gut-brain axis disruption.
Acne, eczema, or psoriasis may correlate with gut inflammation.
Inflammation can manifest outside the gut.
If symptoms persist beyond a few weeks, structured evaluation is recommended.
Not all digestive symptoms indicate structural disease.
Functional disorders like IBS involve:
Inflammatory Bowel Disease involves:
Differentiating between these requires objective testing.
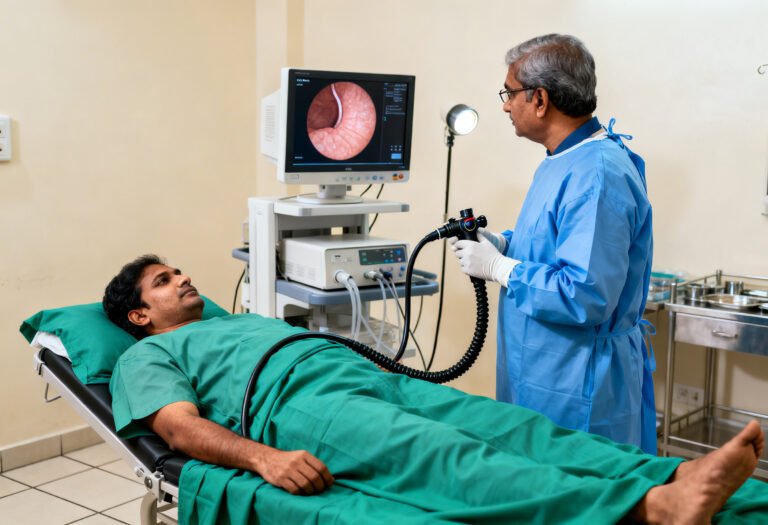
Doctors assess:
Evaluate:
This stool marker helps distinguish inflammatory disease from IBS.
Low levels suggest functional issues. High levels indicate organic inflammation.
Visualize the lining and allow biopsy confirmation.
CT enterography or MR enterography helps evaluate small intestine involvement.
Advanced evaluation is available in structured GI programs including GutHealthDoctor and at Arka Anugraha Hospital in Bengaluru.
Dr. Gaurang Ramesh integrates both conventional and functional assessment strategies when appropriate.
Many patients benefit from structured mucosal healing strategies.
Eliminate:
Support digestion using:
Restore beneficial bacteria through:
Support epithelial regeneration with:
Address:
This step is essential for long-term remission.
When structural inflammation is confirmed:
Surgical options are available for complications such as strictures or fistulas.
Arka Anugraha Hospital provides advanced laparoscopic and minimally invasive surgical care when required.
Indian cuisine contains powerful anti-inflammatory ingredients.
Curcumin supports tight junction integrity.
Improves motility and reduces cytokine signaling.
Rich in Vitamin C and antioxidants.
Supports digestion and bile flow.
May support microbiome balance.
Pair turmeric with black pepper to enhance absorption.

Consult a gastroenterologist if:
Early intervention improves outcomes and reduces risk of complications.
GutHealthDoctor and Arka Anugraha Hospital provide structured evaluation programs in South Bengaluru for patients seeking root-cause assessment.
Maintaining gut resilience requires:
Gut inflammation is reversible in many early-stage cases when addressed systematically.
Inflammation in the gut is not just a digestive issue. It is an immune condition with systemic implications. Early signs such as bloating, fatigue, and bowel irregularity should not be ignored.
With structured diagnostics, integrative management, and lifestyle correction, long-term mucosal healing is achievable.
If symptoms persist, timely consultation helps prevent progression to chronic inflammatory disease.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.