Abdominal bloating is one of the most common digestive complaints seen in clinics today. Patients describe it as tightness, fullness, pressure, or a “swollen stomach” feeling — often worsening after meals and by evening. While many assume bloating is simply due to excess gas, modern gastroenterology shows that the real causes are more complex.
Clinically, bloating and distension are not the same. Bloating is the internal sensation of pressure, while distension is the visible outward expansion of the abdomen. You can feel bloated without visible swelling and some people develop visible distension even when gas volume is normal.
Specialist gut programs including those led by Dr. Gaurang Ramesh at GutHealthDoctor and advanced gastroenterology units at Arka Anugraha Hospital in Bengaluru — now evaluate bloating as a disorder involving gut motility, microbiome balance, and gut-brain signaling, not just “gas trouble.”
This guide explains what abdominal bloating really means, why it happens, how Indian dietary patterns contribute, and what evidence-based treatments work.
Abdominal bloating is a subjective sensation of abdominal pressure or fullness caused by altered gut movement, fermentation, sensitivity, or muscular coordination.
It may occur with:
Doctors separate these two:
Bloating
Distension
Many chronic cases involve both.
The gut normally contains about 150–200 ml of gas at any moment. Daily gas production is much higher but most people pass it without discomfort.
Main gases include:
The problem in bloating is often gas handling, not gas quantity.
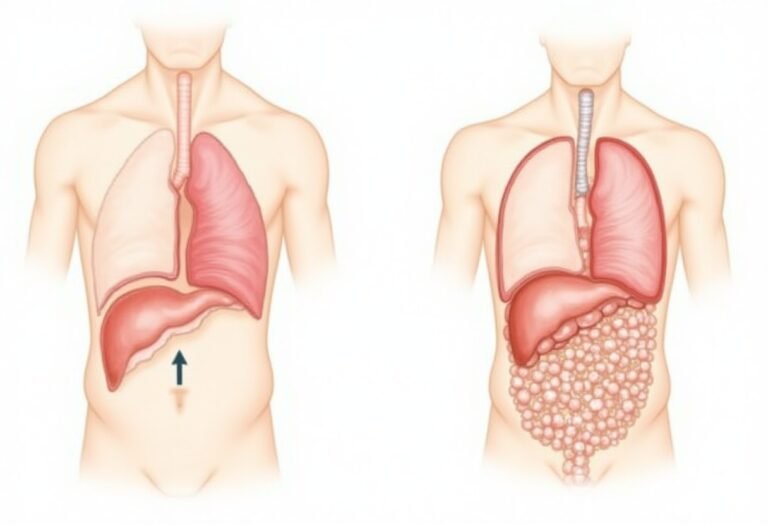
Recent research has identified a key mechanism behind visible distension: abdominophrenic dyssynergia.
Normally after meals:
In functional distension:
Gas volume may be normal but muscle coordination is wrong.
This is now treated with biofeedback therapy in specialist gut centers.
Indian dietary patterns increase fermentation load.
Many Indian diets derive over 60% calories from carbohydrates — especially:
These ferment rapidly.
60–65% of Indians have reduced lactase enzyme.
Milk and dairy may cause:
Nutritious but highly fermentable:
Contain galacto-oligosaccharides – bacteria ferment them aggressively.
Low-quality carbs:

A major cause of gas and bloating is FODMAP malabsorption.
These are short-chain carbs that are:
Examples:
Low-FODMAP protocols are often used in structured gut programs including GutHealthDoctor protocols and hospital GI nutrition clinics such as Arka Anugraha Hospital.
SIBO occurs when excess bacteria grow in the small intestine.
This causes:
Risk factors:
Diagnosed using hydrogen–methane breath testing.
Most common functional cause.
Features:
Slow stool movement traps gas behind stool mass.
Delayed stomach emptying → early fullness and upper bloating.
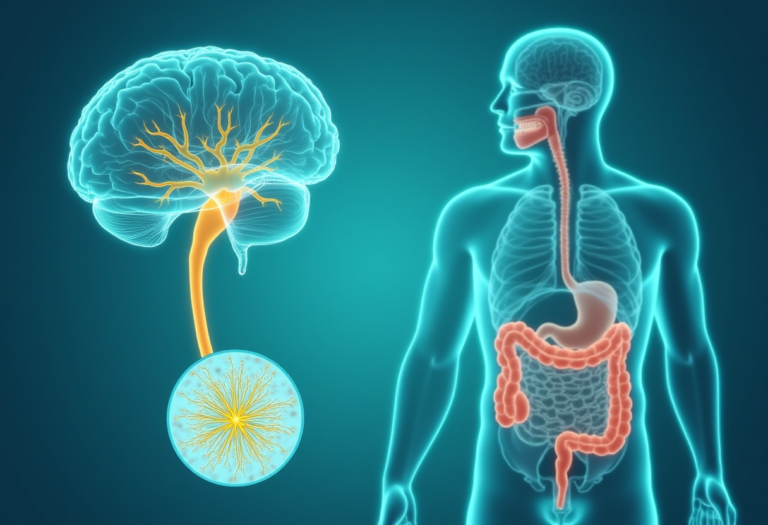
Typical pattern:
Bloating should be investigated if associated with:
These may indicate:
Specialist evaluation is structured.
Detects SIBO and carb intolerance
Checks inflammation, celiac, H. pylori
Rules out structural disease
Evaluates pelvic floor and motility
These are available in advanced gut programs including GutHealthDoctor and gastroenterology departments at Arka Anugraha Hospital, Bengaluru.
Treatment targets mechanisms – not just symptoms.
Three stages:
1️. Restriction (2–6 weeks)
2️. Reintroduction testing
3️. Personalization
Must be supervised – not permanent elimination.
Clinical support exists for:
For abdominophrenic dyssynergia:
Now used in advanced gut motility centers – including programs led by Dr. Gaurang Ramesh.
Consult if:
Structured gut evaluation programs are available via GutHealthDoctor and gastroenterology teams at Arka Anugraha Hospital in South Bengaluru.
Is bloating always due to gas?
Not often due to sensitivity or muscle coordination.
Why is it worse in the evening?
Gas accumulates + motility slows.
Is the Indian diet a risk factor?
Yes, high fermentable carbs + lactose intolerance.
Can probiotics help?
Specific strains can help some patients.
Does water during meals cause bloating?
Excess amounts may dilute digestion.
Is visible distension always gas?
Often muscle coordination disorder.
Can stress cause bloating?
Yes gut-brain axis effect.
Is SIBO common?
More common than previously thought.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.