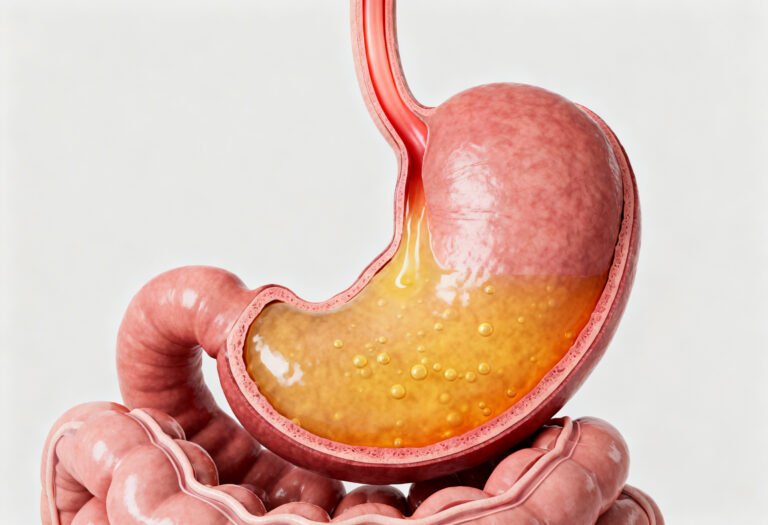
Acid reflux occurs when stomach contents flow backward into the esophagus. The esophagus is the tube that carries food from your mouth to your stomach. At the lower end of this tube is a muscular valve called the lower esophageal sphincter, or LES.
Normally, the LES:
When the LES weakens or relaxes at the wrong time, acid from the stomach moves upward. This acid irritates the lining of the esophagus, which is not designed to tolerate such low pH levels.
This irritation produces the classic burning sensation known as heartburn.
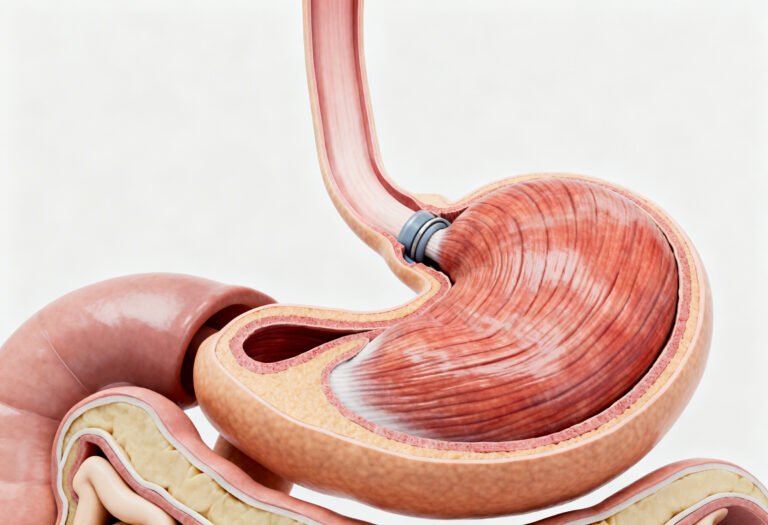
Not every episode of reflux is a disease.
Occasional reflux:
GERD:
If acid exposure persists over time, it can lead to:
This is why persistent symptoms should not be ignored.
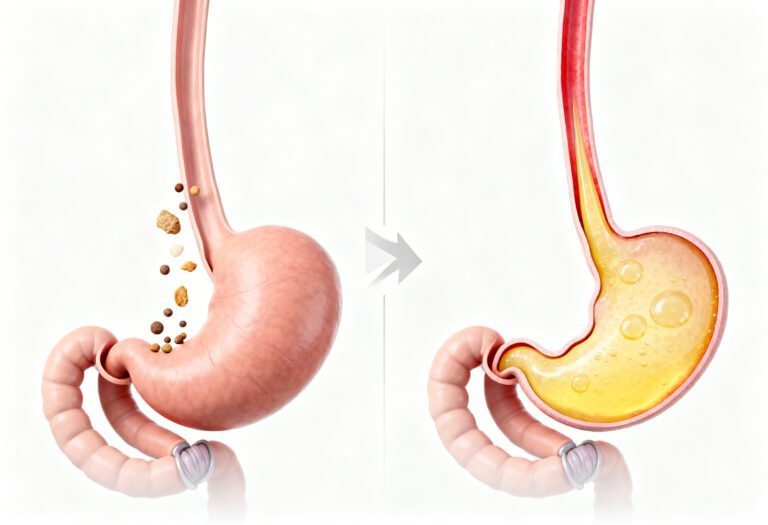
Several lifestyle changes are contributing to rising GERD prevalence in cities like Bengaluru, Delhi, and Mumbai.
Dinner within 2 to 3 hours of sleep increases the risk of nocturnal reflux.
Long hours of sitting increase abdominal pressure and slow digestion.
Abdominal fat increases pressure on the stomach, pushing acid upward.
Frequent consumption of:
All contribute to lower LES pressure and delayed gastric emptying.
Specialist gastroenterology programs such as those at GutHealthDoctor and Arka Anugraha Hospital often see a direct link between lifestyle changes and chronic reflux symptoms.
Acid reflux is rarely caused by a single factor. It usually results from a combination of structural, physiological, and dietary triggers.
Transient relaxations of the LES allow acid backflow even without swallowing.
When part of the stomach bulges through the diaphragm, the natural support system for the LES weakens.
Excess weight increases intra-abdominal pressure.
When food stays in the stomach longer than normal, pressure builds up.
Hormonal relaxation of muscles plus increased abdominal pressure commonly trigger reflux.
Certain food habits common in India increase reflux risk.
Capsaicin can irritate the esophageal lining.
High fat slows gastric emptying.
Caffeine reduces LES pressure.
Gas distension increases reflux risk.
High acidity can aggravate symptoms.
Reflux diet tips often involve identifying personal triggers rather than eliminating all spices permanently.
Typical symptoms include:
Some patients experience extraesophageal symptoms without classic heartburn.
These may include:
This is called Laryngopharyngeal Reflux, or silent reflux.
Immediate evaluation is required if you experience:
These may indicate serious complications.
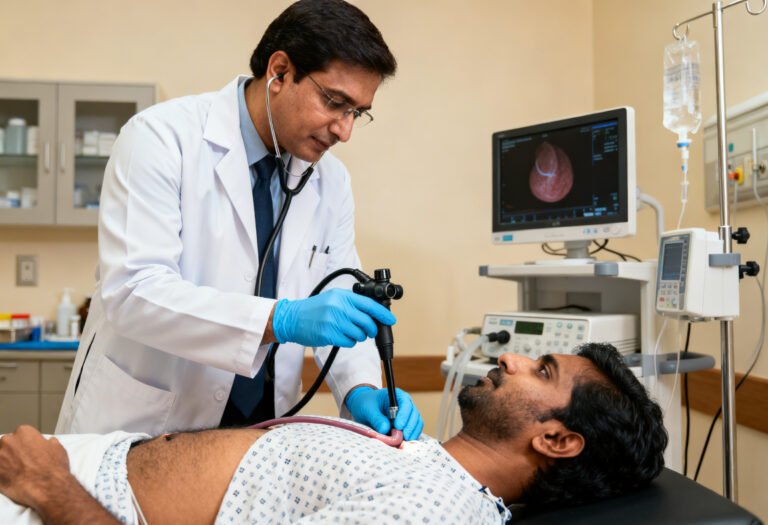
Your doctor evaluates:
An 8-week proton pump inhibitor course may be prescribed.
If symptoms persist or red flags are present, tests may include:
Visualizes inflammation or Barrett’s changes.
Measures acid exposure.
Evaluates esophageal muscle coordination.
These tests are available in structured GI centers including GutHealthDoctor and tertiary hospitals like Arka Anugraha Hospital in Bengaluru.
Treatment depends on severity.
These form the foundation of reflux treatment.
Provide quick relief but short duration.
Reduce acid production for moderate symptoms.
Most effective for healing esophagitis.
Best taken 30 to 60 minutes before breakfast.
Long-term use should be supervised by a specialist.
For patients not responding to medication:
Creates a stronger valve mechanism.
Supports LES closure.
Minimally invasive repair.
These are considered when objective testing confirms significant reflux.
Consult a gastroenterologist if:
Dr. Gaurang Ramesh at GutHealthDoctor follows an integrative reflux evaluation approach, combining conventional testing with functional gut assessment when needed.
Early consultation prevents complications and reduces long-term medication dependence.
During your first visit:
A personalized reflux management roadmap is created, focusing on sustainable recovery rather than short-term suppression.

Long-term prevention requires:
In many patients, a combination of lifestyle change and structured medical supervision provides long-term remission
Not everyone. Triggers are individual and should be identified systematically.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.