Constipation is one of the most common digestive complaints yet one of the most misunderstood. Many people think constipation simply means “not passing stool daily.” In medical reality, constipation includes hard stools, excessive straining, incomplete evacuation, or a feeling of blockage even if bowel movements happen every day.
Across India, especially in urban populations like Bengaluru, chronic constipation is rising due to sedentary lifestyle, low fiber intake, dehydration, stress, and gut brain axis imbalance.
Specialist gut clinics including programs led by Dr. Gaurang Ramesh at GutHealthDoctor and gastroenterology units at Arka Anugraha Hospital now evaluate constipation as a functional and physiological disorder, not just a diet problem.
Let’s understand constipation properly from mechanism to treatment.
Constipation is a condition where bowel movements become:
Medical definitions include:
Modern gastroenterology uses symptom quality, not just frequency, to diagnose constipation.
Primary keyword: constipation
Secondary keywords: chronic constipation causes, hard stool problem
LSI keywords: difficult bowel movement, incomplete evacuation, slow bowel transit
Normal bowel patterns vary:
If stool is hard, painful, or incomplete it is clinically constipation even if daily.
Passing stool is a coordinated neuromuscular process involving:
Colon muscles push stool forward while absorbing water.
If movement is slow → stool becomes dry and hard.
When stool reaches rectum, stretch sensors signal the urge to pass stool.
If urge is repeatedly ignored → signals weaken.
To pass stool:
If muscles tighten instead of relaxing → outlet constipation occurs.
This is called dyssynergic defecation — very common but often missed.
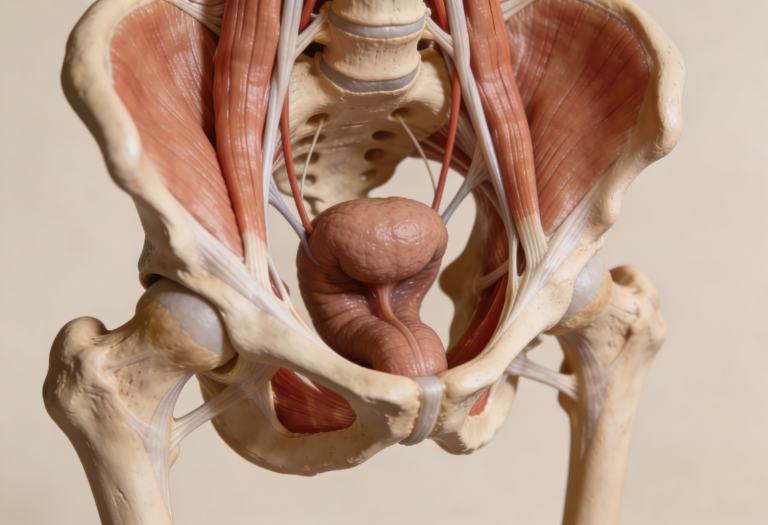
Colon movement is sluggish
Stool dries excessively
Pelvic floor coordination problem
Patient pushes but exit remains closed
Constipation with bloating and abdominal pain
Gut brain axis driven
Due to disease, hormones, or medication
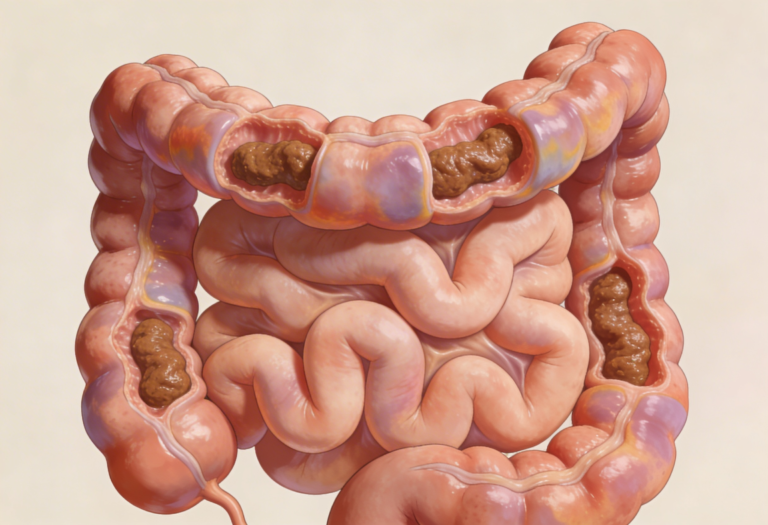
Most common cause in Indian diets today.
Refined foods replacing traditional grains:
Fiber adds bulk and softness to stool.
Fiber without water worsens constipation.
Movement stimulates bowel reflexes.
Desk jobs and long sitting reduce gut motility.
Repeated suppression causes rectal desensitization.
Common in:
Stress suppresses digestive nerve activity and slows bowel movement.
Very common and often overlooked:
Methane-producing microbes slow gut transit significantly.
Often seen with:
Specialist testing may be required commonly done in advanced gut programs including GutHealthDoctor and tertiary GI centers such as Arka Anugraha Hospital.
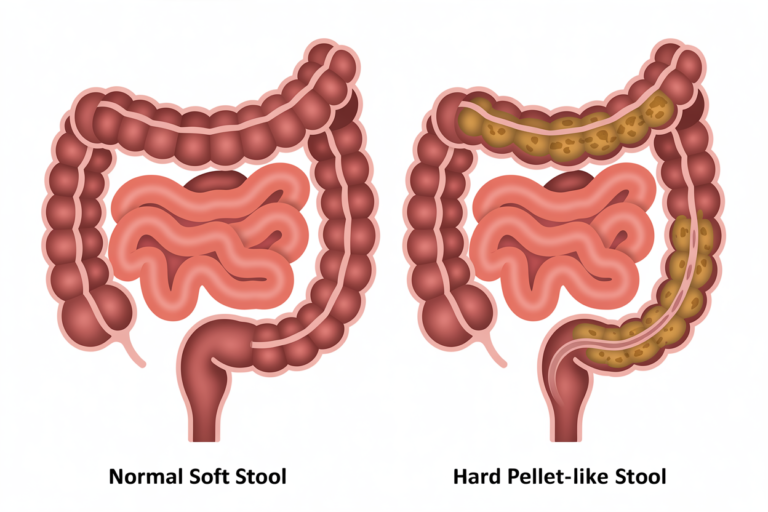
Constipation usually shows:
Ideal stool = Type 3–4.
Do not ignore constipation if accompanied by:
These require colon evaluation.
Specialist evaluation goes beyond diet advice.
Checks:
Measures muscle coordination
Checks evacuation ability
Measures stool movement speed
Visualizes pelvic floor mechanics
Detects methane SIBO
These are available in specialist gut motility centers including GutHealthDoctor programs and hospital GI labs such as Arka Anugraha Hospital
Treatment depends on type, not one-size-fits-all.
Target: 25–30g/day
Indian high-fiber foods:
Effective soluble fiber
Must take with water
2.5–3 liters daily
Warm morning water helps bowel reflex.
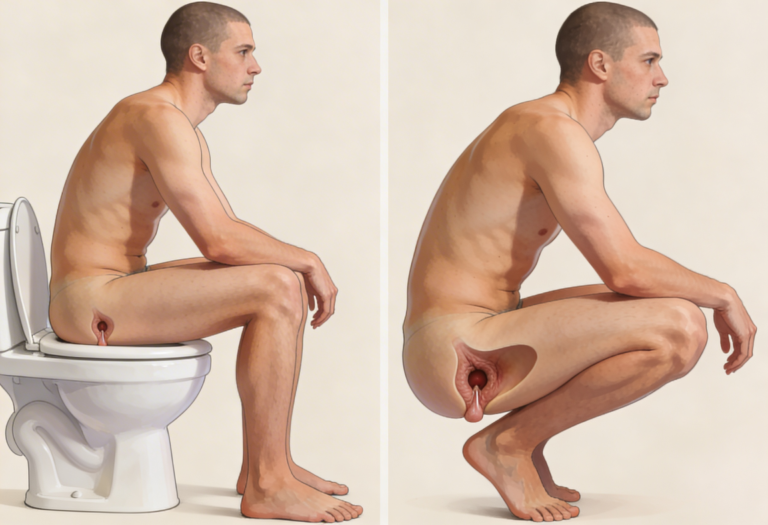
Squatting position is anatomically superior.
Use a footstool on western toilet.
Daily walking improves gut motility.
Draw water into stool
Safe for longer use
Used short-term
Not for chronic daily use without supervision
Used in chronic refractory constipation
Best treatment for outlet obstruction.
Pelvic muscles are retrained using sensor feedback.
Success rates >70%.
Often recommended by gut motility specialists including programs under Dr. Gaurang Ramesh
Consult if:
Structured constipation evaluation is available through GutHealthDoctor and gastroenterology teams at Arka Anugraha Hospital.
Is Isabgol safe daily?
Yes with enough water.
Can constipation cause piles?
Yes straining is main cause.
Does water alone cure constipation?
Only when fiber intake is adequate.
Are laxatives addictive?
Stimulants can be if overused.
Can stress cause constipation?
Yes via the gut-brain axis.
Is squatting better than sitting?
Yes, it improves anorectal angle.
Can probiotics help?
Sometimes strain dependent.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.