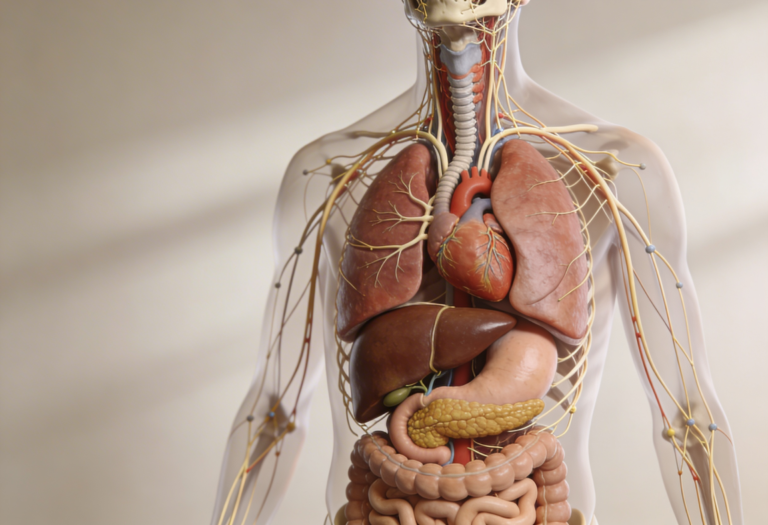
Many people experience digestive symptoms that worsen with stress bloating before meetings, nausea during anxiety, constipation during emotional strain, or sudden urgency during panic. These are not “just in your head.” They are mediated by a real biological pathway called the vagus nerve.
The vagus nerve is the main communication line between the brain and the digestive system. It carries signals that control stomach acid, gut movement, inflammation control, enzyme release, and even how relaxed your intestines are after a meal.
When vagus nerve function is reduced, digestion becomes inefficient, gut sensitivity increases, and symptoms such as IBS, reflux, slow digestion, and functional dyspepsia become more likely.
Specialist gut programs including those led by Dr. Gaurang Ramesh at GutHealthDoctor and gastroenterology teams at Arka Anugraha Hospital in Bengaluru increasingly evaluate vagus nerve and gut-brain axis function when routine digestive treatment does not work.
Let’s understand this in simple clinical terms.
The vagus nerve is the tenth cranial nerve and the longest nerve of the parasympathetic nervous system responsible for “rest and digest” functions.
It starts in the brainstem and travels down through:
It regulates:
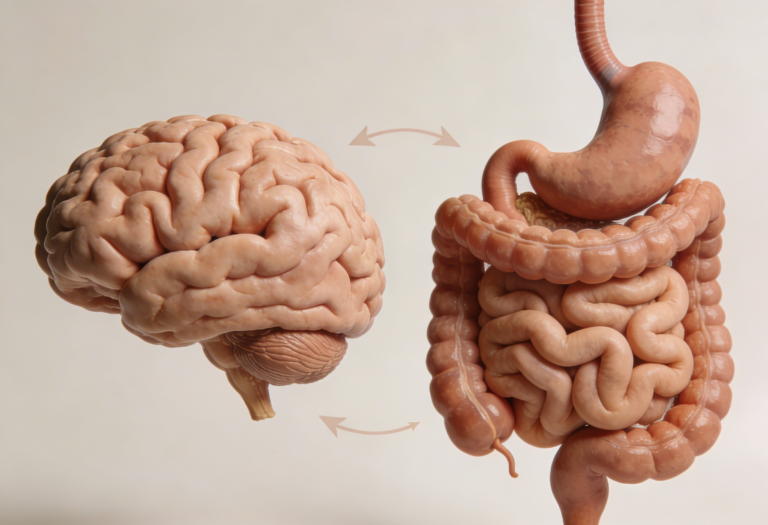
The gut and brain are connected through a bidirectional network called the gut brain axis.
About 80% of vagus nerve fibers are sensory carrying information from the gut upward to the brain.
They transmit signals about:
Only about 20% of signals travel downward from brain to gut to control movement and secretion.
This means your brain constantly monitors your gut status.
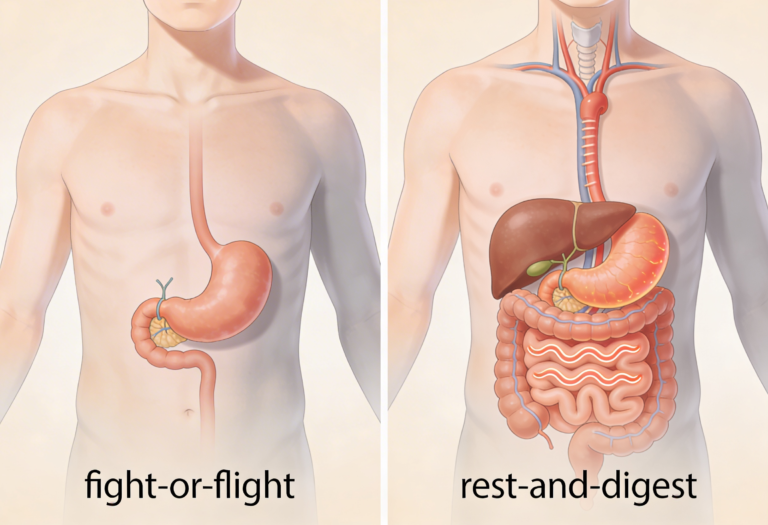
The autonomic nervous system has two modes:
The vagus nerve is the main parasympathetic nerve controlling digestion.
If vagal tone is low, digestion suffers.
Vagal tone refers to how strong and responsive the vagus nerve is.
High vagal tone is associated with:
Low vagal tone is linked with:
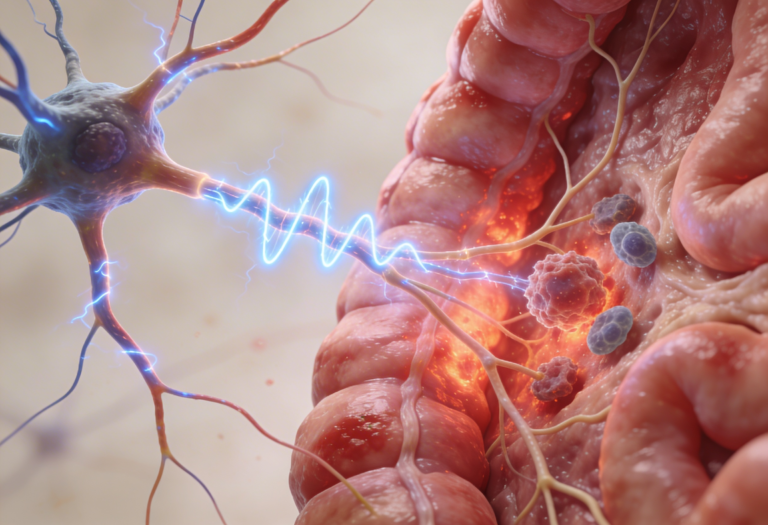
One of the most important vagal functions is the cholinergic anti-inflammatory pathway.
When gut inflammation rises:
This is the body’s built-in inflammation control system.
Reduced vagal signaling is associated with:
Long-term stress suppresses vagal activity and keeps the body in sympathetic mode.
Common in:
Healthy bacteria produce metabolites that stimulate vagal signaling.
Poor diet high in processed foods and sugar reduces these signals.
Traditional Indian fermented foods like curd, idli batter, and buttermilk support this pathway.
After food poisoning or viral gastroenteritis, some patients develop persistent gut brain signaling problems often labeled post-infectious IBS.
Diabetic autonomic neuropathy can directly damage vagus nerve fibers.
Structural factors
Because the vagus nerve controls multiple organs, symptoms are wide ranging.
Patients with combined gut and stress symptoms are often evaluated in gut brain clinics such as GutHealthDoctor and hospital-based integrative GI programs including Arka Anugraha Hospital.
Seek specialist care urgently if you have:
strong family history of GI cancer
Best clinical indicator of vagal tone.
Higher HRV = stronger vagal activity.
Motility testing
Breath testing
Used to detect SIBO and fermentation disorders linked with poor motility.
Some integrative programs use multi-factor gut assessment models that examine:
Treatment focuses on neuro-digestive restoration, not just symptom control.
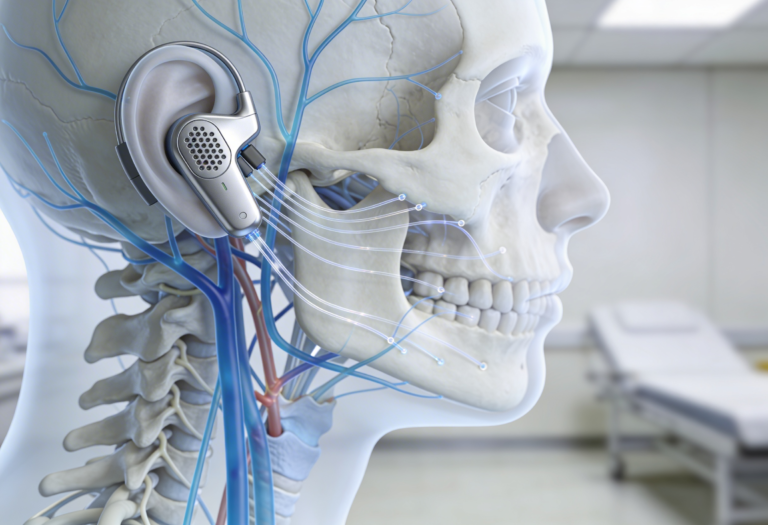
Non-invasive transcutaneous VNS devices stimulate vagal fibers through the ear or neck.
Clinical studies show benefit in:
Structured VNS protocols are used in specialist programs including those supervised by Dr. Gaurang Ramesh.
Targeted probiotics
Certain strains called psychobiotics influence vagal signaling.
Slow breathing stimulates vagus nerve reflexes.
Clinically validated for IBS symptom reduction.
Vocal vibration stimulates vagal fibers in the throat.
Doctors may use:
These are used strategically, not permanently in most cases.
Consult if:
Programs at GutHealthDoctor and Arka Anugraha Hospital offer structured gut-brain axis evaluation pathways.
Can stress damage digestion through vagus nerve?
Yes chronic stress suppresses vagal activity.
What is vagal tone?
Strength of vagus nerve response.
Can breathing exercises help digestion?
Yes proven vagal activation method.
Is VNS safe?
Non-invasive VNS is generally safe.
Can probiotics affect the vagus nerve?
Yes via microbiome metabolites.
Is IBS a gut-brain disorder?
Yes classified as gut-brain interaction disorder.
Is testing available in Bengaluru?
Yes tertiary GI centers provide it.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.
Lorem ipsum dolor sit amet, consectetur adipiscing elit.